This website uses cookies to ensure you get the best experience on our website. Learn more

Hepatocellular carcinoma and advanced liver disease comprise a major public health burden for which we have only unsatisfactory treatment options. According to the European Association for the Study of the Liver (EASL), the prevalence of liver diseases is ~6% in the EU (29 million individuals) and the associated mortality rate was estimated at 14.3 per 100,000 (70,000 deaths/year). HCC is the third most common cause of cancer-related death and the leading cause of death among cirrhotic patients. According to the EASL, the HCC incidence and mortality rates were of 65,000 and 60,240 cases in Europe, respectively. Given the growing incidence of HCC, the economic burden will significantly increase in Western populations during the next decades. Treatment options for liver steatosis, fibrosis, cirrhosis and HCC are unsatisfactory. Furthermore, there are no efficient chemopreventive strategies to limit HCC development once cirrhosis is established. Although early-stage tumors can be curatively treated using surgical approaches, they are often undiagnosed and treatment options for advanced HCC are unsatisfactory. Although the multikinase inhibitor sorafenib improves a survival benefit for patients with locally advanced or metastatic HCC, adverse effects and moderate efficacy limit its use in patients with advanced liver disease. Thus, a therapy that is well tolerated, cost-effective, and poses an acceptable risk-to-benefit ratio is missing.
Virus-induced chronic hepatitis is a leading cause of HCC in France and Europe. In the developed Western world, only 10-15% of cases can be attributed to hepatitis B virus (HBV) infection, while chronic hepatitis C appears to be the major risk factor for HCC (up to 70% of cases) in Europe. Importantly, there are common alterations of pathways that likely account for viral and non-viral pathogenesis regardless of their etiology.
Unsatisfactory therapeutic options are due too several hurdles:
Given these hurdles there is a need for better understanding of pathogenesis of HCC, discovery of novel targets and better animal models for study of hepatocarcinogenesis and preclinical evaluation of therapeutic approaches. Further given the genetic heterogeneity of HCC and their origin in advanced liver disease and cirrhosis, it is of paramount interest to develop individualized treatment approaches and clinical care needs to integrate management of advanced liver disease using surgical and medical approaches.
CNRS U7504, University of Strasbourg
DHU AP-HP, Beaujon Hospital, University of Paris VII
Inserm U1110, IHU, LabEx HepSYS Strasbourg, Strasbourg University Hospitals
Inserm U674, Hopital Européen Georges Pompidou, Université Paris Descartes,
Inserm U1121, University of Strasbourg
PHENOMIN- Institut Clinique de la Souris, CNRS UMR7104 / INSERM U964 / University of Strasbourg
UMR 7006, University of Strasbourg
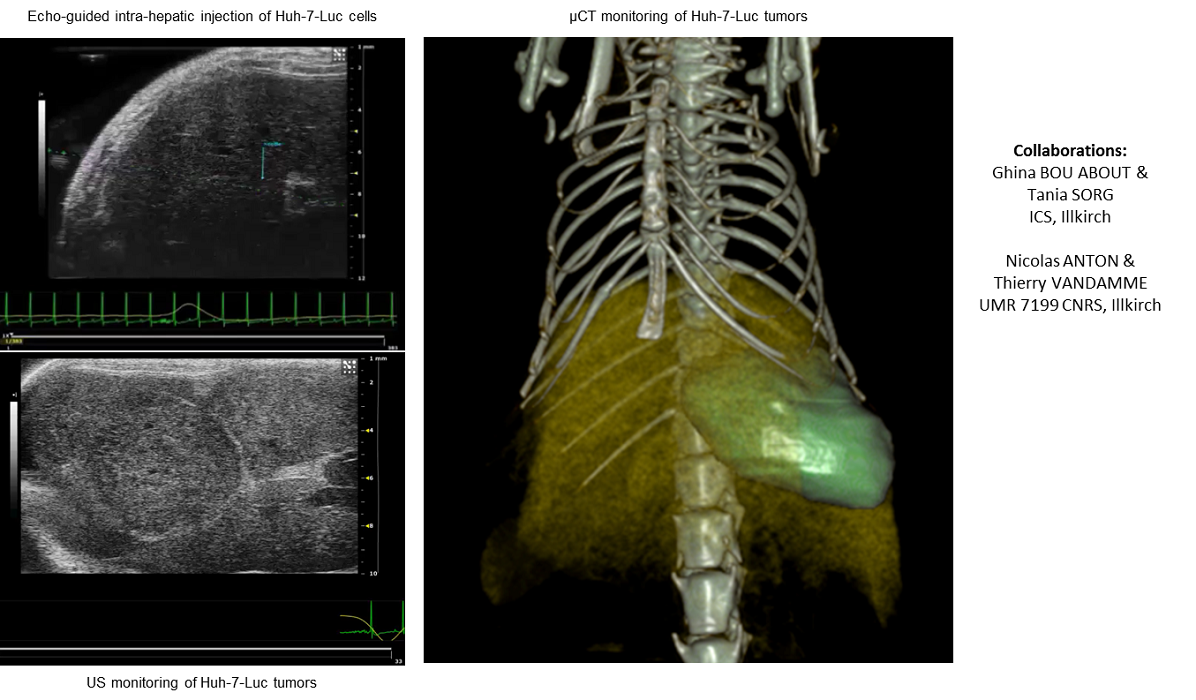
Ultrasound (US) image-guided orthotopic injection of human HCC tumor cells in the liver parenchyma has been set-up and validated at the Clinical Mouse Institute. In a first series of experiments, US image-guided mini-invasive injection of Huh-7 cells in immunodeficient mice was successfully performed, leading to tumor engraftment (monitored monitored by echography, micro-CT, bioluminescence imaging and histology) in the targeted hepatic lobe (Fig. 1) with a similar efficacy as after injection under laparotomy. Evaluation of US-imaging guided intra-tumoral injection of drugs nanovectors is now underway at the Mouse Clinical Institute. The use of US imaging for intra-hepatic or intra-tumoral injections allows to refine this model, in agreement with the 3R’s rules of animal experimentation.
3Rs rules in animal experimentation
The development of multimodal strategies for the treatment of hepatocellular carcinoma requires tractable animal models allowing for advanced in vivo imaging. Here, we characterize an orthotopic hepatocellular carcinoma model based on the injection of luciferase-expressing human hepatoma Huh-7 (Huh-7-Luc) cells in immunodeficient mice. Luciferase allows for an easy repeated monitoring of tumor growth by in vivo bioluminescence. The intrahepatic injection was more efficient than intrasplenic or intraportal injection in terms of survival, rate of orthotopic engraftment, and easiness. A positive correlation between luciferase activity and tumor size, evaluated by Magnetic Resonance Imaging, allowed to define the endpoint value for animal experimentation with this model. Response to standard of care, sorafenib or doxorubicin, were similar to those previously reported in the literature, with however a strong toxicity of doxorubicin. Tumor vascularization was visible by histology seven days after Huh-7-Luc transplantation and robustly developed at day 14 and day 21. The model was used to explore different imaging modalities, including microtomography, probe-based confocal laser endomicroscopy, full-field optical coherence tomography, and ultrasound imaging. Tumor engraftment was similar after echo-guided intrahepatic injection as after laparotomy. Collectively, this orthotopic hepatocellular carcinoma model enables the in vivo evaluation of chemotherapeutic and surgical approaches using multimodal imaging.
Download the publicationHepatocellular carcinoma (HCC) is the second leading cause of cancer death worldwide. While curative approaches for early stage HCC exist, effective treatment options for advanced HCC are lacking. Furthermore, there are no efficient chemopreventive strategies to limit HCC development once cirrhosis is established. One challenge for drug development is unsatisfactory animal models. In this article, we describe an orthotopic xenograft mouse model of human liver cancer cell lines through image-guided injection into the liver. This technique provides a less invasive yet highly efficient approach to engraft human HCC into mouse liver. Similarly, image-guided injections are used to deliver chemotherapeutics locally, enabling reduction in potential systemic adverse effects, while reducing the required dose for a therapeutic effect. In summary, this image-guided strategy provides a novel and convenient approach to improve current HCC mouse models. © 2019 The Authors. This is an open access article under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs License, which permits use and distribution in any medium, provided the original work is properly cited, the use is non-commercial and no modifications or adaptations are made.